Is the BCRAT Screening Tool Olivia Munn Used Right for Everyone?
With this information in mind, why doesn’t everybody complete the BCRAT to determine their breast cancer risk score? Some evidence shows that the BCRAT might not provide complete or accurate data for all demographics.
For example, it was originally developed in 1989 based on data only from white women. However, the algorithm has been updated to increase screening accuracy in women of Black, Hispanic, Asian, and Pacific Islander descent. The NCI stated that it could underestimate risk in Hispanic women born outside the U.S. and in Black women with previous biopsies. The site suggests that more research is needed to validate risk in various subgroups.
In addition, while the BCRAT tends to under-represent risk, a standard screening counterpart used by healthcare providers called the International Breast Cancer Identification Study (IBIS) tends to over-represent risk. Doctors may balance both screens to identify at-risk patients.
The BCRAT also may not be the ideal tool for patients with a history of the following medical conditions:
- Breast cancer or Lobular Carcinoma in Situ (LCID) or Ductal Carcinoma in Situ (DCIS)
- Past radiation treatment of the chest
- Known BRCA1 or BRCA2 gene mutations
- Other rare breast cancer-causing syndromes (for example, Li-Fraumeni Syndrome)
What About Other Screening Tools, Risk Calculators, and Diagnostic Methods?
The National Comprehensive Cancer Network (NCCN) contains valuable resources for patients and caregivers about various cancer-related topics and screening options. Other breast cancer screening tools also exist beyond the BCRAT risk calculator, although enough evidence may not exist to say definitively which resource is best.
Available tools or strategies include:
Having accurate screening tools ensures the right people receive referrals for additional testing. The existing limitations of specific diagnostic modalities further highlight this importance. In addition to genetic considerations, the NCI discusses in greater detail the benefits and harms of various additional breast cancer assessment and diagnostic methods:
- Screening with Mammography
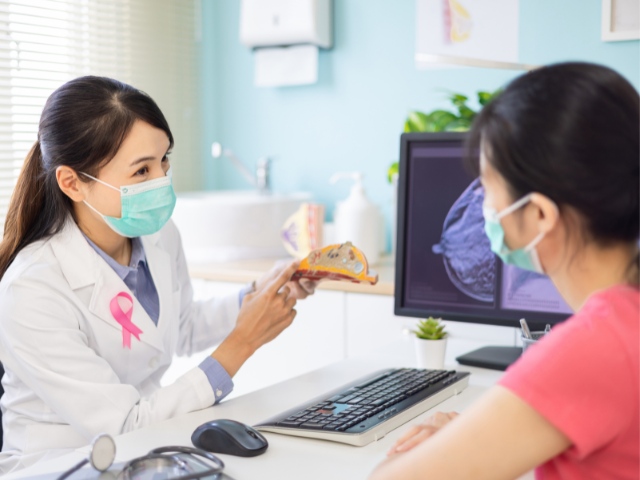
- Clinical Breast Examination (CBE)
- Breast Self-Examination
- Mammography adjuncts (secondary screening tools)
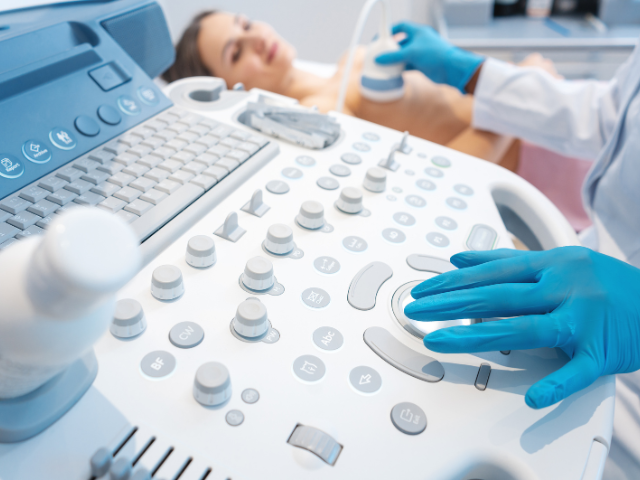
- Ultrasound
- MRI
- Thermography
Of note is that the majority of those who get breast cancer do not have a genetic predisposition.
“Only 5 to 10% of people who get breast cancer have a gene that tests positive,” Joann Mortimer, MD, medical oncologist, and Women’s Cancers Program director, said.
Also, 17% to 43% of women with cancer have a falsely negative clinical breast examination (CBE). Finally, breast self-examination (BSE) has been found to have no definitive reduction in mortality compared to no BSE.
Keep in mind that tests like mammography are imperfect. Essential mammograms tend to miss tumors in dense breast tissue. Women with dense breast tissue – about half of women older than 40 – have a higher proportion of glandular and fibrous tissue, making it harder to identify the cancer. Essential mammography screening can cause false negatives due to invasive breast cancers being undetected in 6% to 46% of cases.
On the other hand, routine mammography screening results in 10% of women being recalled for further testing. These false positives can cause unnecessary anxiety and testing.

Role of Nurses in Breast Cancer Prevention
Nurses can advocate for preventive and proactive healthcare, including awareness of cancer screening resources. According to a Gallup ethics poll, in 2023, nurses earned the topmost trusted spot of surveyed professions for the 22nd year. The general public consistently trusts nurses more than any other profession.
Often, they also count on nurses to be aware of trends in public health issues and the diagnosis and treatment of illnesses. Nurses can also point friends, family members, or patients to their doctors for these complex discussions.
Following Munn’s announcement, an NCI spokesperson claims visits to the BCRAT tool website have increased dramatically. What does this heightened awareness surrounding cancer risk tools mean for nurses, patients, and the public? Understanding the accuracy of existing information and recommendations is crucial. Unfortunately, even following routine physician-recommended cancer screenings may not always result in a timely or accurate breast cancer diagnosis.
A more proactive and multifaceted approach is sometimes needed. Munn’s experience sheds light on the need for additional screening action and further research into existing methods to increase effectiveness across all demographics.