Events | Holidays & Freebies National Nurses Week: Honoring Our Favorite Pop Culture Practitioners National Nurses Week runs from May 6-12, and includes a variety of ways to honor nurses. This year’s theme is “Nurses Make the Difference.” As part...


Pharm D
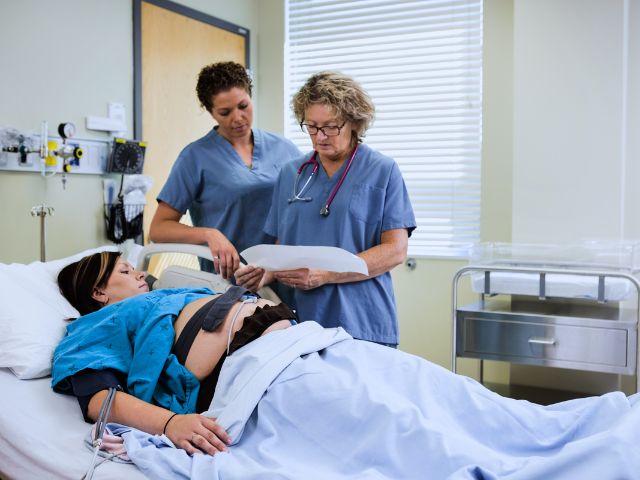
February 2024 is International Prenatal Infection Prevention Month. Let’s discuss the role of nurses in the prevention of prenatal infections.
Prenatal infections, also known as maternal infections, are those transmitted from the mother to the fetus during pregnancy or delivery. According to the WHO, in 2020, every day, almost 800 women die from preventable causes related to pregnancy and childbirth- an unacceptably high number.
Neonatal infections remain a major contributor to the global burden of diseases, with an estimated 6.9 million incident cases of presumed severe neonatal infections each year, causing approximately half a million deaths worldwide in 2012.
Some prenatal infections can lead to the deaths of the fetus or the mother, while others can lead to lifelong disabilities in the child. Therefore, healthcare providers need to play a role in preventing prenatal infections.
Nurses are the backbone of the healthcare industry and play a pivotal role in prenatal infection prevention as they counsel the patient, take a detailed medical history, and diagnose the infection before it spreads.
The three common types of gynecological infections that can be life-threatening for the mother and the fetus are toxic shock syndrome, sexually transmitted infection, and pelvic inflammatory disease.
TSS, or toxic shock syndrome, is a life-threatening condition caused by the strains of Staphylococcus aureus that produce toxins leading to coagulation disorder and shock. If these toxins enter the bloodstream, they can also cause tissue damage, leading to organ damage. Toxic shock syndrome occurs when the bacterial load in the reproductive system is too high for a long time.
STIs or sexually transmitted infections are those that spread from one person to another through sexual contact. However, they can also be transmitted through other routes. The most common causative agent for STIs is the Human Papillomavirus, having more than 100 variants.
PID, or pelvic inflammatory disease, is an infection of the upper reproductive tract, commonly occurring because of asymptomatic STIs. Areas of the reproductive tract, such as the cervix, uterine cavity, fallopian tubes, and pelvic cavity, are involved. It can also result in infertility.

Nurses play an essential role in educating and counseling women about maintaining vaginal hygiene to prevent sexually transmitted infections. As a nurse, be nonjudgmental, identify high-risk behaviors, and provide sensitive counseling in every prenatal visit to your patients.
To prevent a prenatal infection and to detect it early before it spreads, the following nursing interventions can be helpful.
A complete medical history is essential to rule out if the patient is at risk of developing a prenatal infection. Make sure to take a detailed medical history and ask if the patient has multiple sexual partners or has a past or recent history of intercourse with bisexual men, as it increases the risk of HIV/AIDS and STIs.
Inform your patient that sexually transmitted infections are transmitted from one person to another through sexual contact.
Take the history of the recent travel and cultural background of the patient. Review the patient’s lifestyle and profession to have an insight into the associated risk factors.
Pay special attention to adolescents, especially those not having a supportive family background, as they may lack information about preventing sexually transmitted infections. Almost half of STIs occur in adolescents.
Assess the patient for specific signs and symptoms of STIs and other infections and notify the physician if you notice any. Check them for any warts or visible lesions and inquire about urinary frequency, cloudy or foul-smelling urine, dysuria, and changes in urine color. Also, ask about vaginal discharge, its consistency, and color.
Identifying the symptoms helps in diagnosing the condition and devising the appropriate treatment. Some organisms have a preference to attack the fetoplacental unit and the neonate. Although the mother may be asymptomatic, organisms such as Mycoplasma and Ureaplasma affect many pregnant women and show up in aborted fetuses.
Detecting visible lesions and warts can help diagnose Herpes Simplex virus type II or Condyloma, which can be transmitted to the neonate at the time of delivery if the mother has a visible lesion present at the time of birth or viral shedding is going on.
Escherial coli or Group B streptococcus can cause urinary tract infections. However, sometimes the patient might be asymptomatic. A sexually transmitted infection may show up as foul-smelling vaginal discharge with discoloration and excessive amounts.
Differentiating between an STI and a UTI in women can be difficult sometimes. A detailed history of the patient and lab reports can help diagnose and differentiate between them.
Know if the infection is primary or recurrent. Herpes Simplex virus and Cytomegalovirus, both recur when the body is under stress. However, only primary cytomegalovirus is problematic to the fetus, and 50% of the exposed fetuses are affected by it.
Moreover, if a newborn is exposed to visible lesions of Herpes Simplex virus II at the time of delivery, they can be affected, resulting in a severe life-threatening systemic infection.
Check the status of the maternal membranes. If they are ruptured, keep an eye on blood cell count and fetal heart rate. Also, check the vagina for any discharge with odor.
Chlamydia, mycoplasmas, and Ureaplasma urealyticum are often transmitted through the ascending route and develop bacteremia, pneumonia, or possibly meningitis. Chlamydial infections can lead to premature rupture of membranes, preterm labor, and endometritis in the postpartum stage.
Neonates born while the mother has a chlamydial infection can develop conjunctivitis or pneumonia after birth.
Comprehensive STI screening is essential as it indicates the risk for HIV acquisition and transmission that is common among men who are involved in sexual activities with other men. People seeking treatment or getting evaluated for other sexually transmitted infections should be screened for HIV and other STIS depending on the community prevalence and individual risk factors. Educate your patient about the tests being conducted for STI screening and explain why they are necessary.
Inserting anything foreign inside the body can become a hub of infections. Inform your patients that the wrong use of tampons, diaphragms, and cervical caps can even lead to toxic shock syndrome and organ damage.
Encourage your clients to wash their hands thoroughly with soap and water before inserting anything foreign inside the body and to change tampons every 4 hours. They should not be used during sleep when possible.
The need to highlight the appropriate use of tampons and other sexual devices is essential. Patients may not understand the serious consequences, such as toxic shock syndrome, organ damage, or even amputation; therefore, as a nurse, educate your patients about tampon use and other devices.
The best practice to prevent a sexually transmitted infection while being sexually active is to use condoms during sexual intercourse as they prevent infection transmission. Other measures can also help, such as using the restroom and washing the genitals after sexual activity.
Ensure your patients understand the necessity of using protection, especially when engaging in sexual activity with multiple partners. People may transmit STIs without ever knowing they have one.
Adolescents need special attention on safe sex practices. Educate them about condom use and the importance of health screening for STIs- that remains an essential part of nursing responsibility.
Informing your patients about vaccines against sexually transmitted infections and getting them administered is essential in preventing their transmission. Immunization against human papillomavirus not only reduces the chances of HPV infection but also reduces the rate of cervical and penile cancer. Hepatitis B vaccine can prevent the occurrence of hepatitis B virus, and immunoglobulin can be administered if known exposure has occurred.
Educating patients about the disadvantages of douching is essential. Douching leads to changes in the internal genital flora and predisposes the patient to develop pelvic inflammatory disease, ectopic pregnancy, and vaginosis.
Many patients believe that regular douching is a part of cleansing. But as a nurse, you should educate the patient to avoid douching to prevent pelvic inflammatory disease.
Educating the patient on preventing toxoplasmosis is essential. Encourage pregnant patients to avoid consuming undercooked meat and not to change a cat litter box or garden in the soil in an area where cats may defecate to avoid exposure to the disease. Reinforce proper hand washing after handling uncooked meat.

Antibiotics and other medications are required to prevent and lower the incidence of sexually transmitted diseases.
To alleviate its symptoms and for its treatment, antibiotics are required, such as azithromycin, doxycycline, erythromycin, ceftriaxone, and benzathine penicillin G; antivirals such as acyclovir; and antifungals such as miconazole, clotrimazole, or fluconazole. For treating Gardnerella infections, bacterial vaginosis and trichomonas, metronidazole and tinidazole can be of help. Prescribe antibiotics accordingly, to which the organism is sensitive.
Nurses may also need to prepare the patient for termination of pregnancy. That time can be very challenging for parents, especially for the mother. Be supportive and empathetic towards them.
Nurses play an essential role in prenatal infection prevention. Be nonjudgmental while you take a complete medical sexual history. Help patients protect themselves with this guide for International Prenatal Prevention Month 2024!
Love what you read?
Share our insider knowledge and tips!
Read More

Events | Holidays & Freebies National Nurses Week: Honoring Our Favorite Pop Culture Practitioners National Nurses Week runs from May 6-12, and includes a variety of ways to honor nurses. This year’s theme is “Nurses Make the Difference.” As part...
Events National Cancer Prevention Month February is National Cancer Prevention Month 2024! Nurses can be an educational resource for patients on how to protect themselves. Cancer prevention can look like lifestyle changes to minimize modifiable risk factors and...

Events World Diabetes Day 2023 November 14th is World Diabetes Day, a time to reflect and deepen our understanding of a nurse’s role in patients’ diabetic care. Review the types of diabetes, risk factors that increase the chance of diabetes, the...