Events | Holidays & Freebies National Nurses Week: Honoring Our Favorite Pop Culture Practitioners National Nurses Week runs from May 6-12, and includes a variety of ways to honor nurses. This year’s theme is “Nurses Make the Difference.” As part...


Pharm D
Diabetes mellitus is a global epidemic, with people with it exceeding 366 million. November 14 is world diabetes day. Let’s talk about it.
According to the WHO, 422 million people have diabetes worldwide, and 1.5 million deaths are attributed to it each year. Moreover, according to the CDC, and Centers for Disease Control and Prevention, 1 in 10 people in the US is living with diabetes, which is around 37.3 million Americans. In the US, 1 in 5 people have diabetes, and they don’t know about it. Moreover, of 96 million American adults, more than 1 in 3 have prediabetes.
Diabetes mellitus is a chronic metabolic disorder in which the blood glucose levels remain high. Left untreated for a long time, it can lead to serious damage to the heart, eyes, kidneys, blood vessels, and nerves, leading to complications such as coronary artery disease, peripheral vascular disease, hypertension, retinopathy, renal failure, and neuropathy that can affect the peripheral nerves, resulting in numbness and pain of the hands or feet.
If glycemic control is poor, there is a high risk of infections because the presence of elevated glucose levels in the blood encourages bacterial growth. The combination of peripheral neuropathies with numbness of the extremities, peripheral vascular disease leading to poor tissue perfusion, and the risk for infection makes the diabetic patient prone to feet and leg ulcers that can even lead to amputation. Therefore, preventing and controlling infections is a must in diabetic patients.
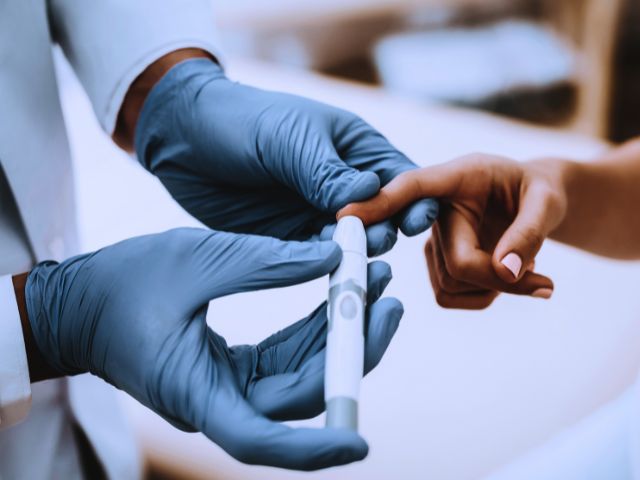
Broadly, diabetes can be classified into two categories, type I and type II diabetes. Other types include gestational diabetes, or diabetes secondary to other conditions such as pancreatic disease, hormonal disease, insulin resistance, or drug-induced.
In type I DM, the beta cells of the pancreas that secrete insulin get destroyed due to an autoimmune reaction, leading to no insulin secretion. Patients with type I diabetes mellitus are lifetime dependent on insulin from external sources to lower blood glucose levels or prevent ketosis.
Therefore, it is also referred to as insulin-dependent diabetes mellitus. Often, it occurs before 20 years and is common in young people. Type I DM can’t be prevented even with a healthy lifestyle. It happens when the beta cells of the pancreas have insulitis, a pancreatic inflammatory response accompanied by beta cell destruction.
Type II diabetes mellitus occurs because of relative insulin deficiency accompanied by resistance to the actions of insulin in muscle, fat, and liver cells. Insulin resistance is also accompanied by increased levels of free fatty acids in the blood, reduced glucose transport in muscle cells, elevated hepatic glucose production, and increased breakdown of fat.
Patients with type II DM are not completely dependent on insulin. But sometimes, they have to administer insulin to maintain glycemic control. Furthermore, they have to take medicines that help sensitize the cells resistant to the action of insulin.
The exact cause of diabetes mellitus is not known, but genetic, autoimmune, viral, environmental, and socioeconomic factors play a role in the development of the disease.
In type I diabetes mellitus, following the environmental stimulus, such as a virus or bacteria, antibodies attack the beta cells of the pancreas and cause insulitis- inflammation and destruction of the beta cells.
The risk factors leading to type II diabetes are:
Diabetes mellitus is diagnosed through blood tests, such as:
The diagnosis of diabetes mellitus is confirmed when fasting plasma glucose is greater than or equal to 126 mg/dL on two occasions or random glucose is greater than or equal to 200 mg/dL along with the classic symptoms of diabetes mellitus such as polyuria, polydipsia, polyphagia, weight loss.
The goal of treatment is to lower and maintain blood glucose levels into the well-controlled range, such as preprandial blood glucose levels of 90– 130 mg/ dL and HbA1c levels of less than 7%.

To manage diabetes the goal is to keep plasma glucose level under control to prevent the delay of complications. Patients having type I diabetes mellitus need subcutaneous insulin. However, in patients with type II diabetes, oral hypoglycemics may be enough. But sometimes, they also need insulin to keep their blood glucose levels under control.
Moreover, with strict dietary adherence to control blood glucose, obese patients with type 2 DM also need weight reduction. The dietitian selects an appropriate calorie allotment depending on the patient’s age, body size, and activity level. Physical activity can also help play a role in reducing blood glucose levels by increasing cellular sensitivity to insulin, improving tolerance to glucose, and encouraging weight loss.
Pharmacological treatments for diabetes include insulin and oral hypoglycemic drugs. They can be described as:
Insulin– is a protein hormone, and its dose varies for each patient as it is titrated to keep the blood glucose levels up to 80 to 140 mg/dL.
The duration of action of insulin varies according to the type.
Oral hypoglycemic agents include sulfonylureas, alpha-glucosidase inhibitors, biguanides, thiazolidinediones, and incretin mimetics.
The dose for antidiabetic drugs varies from patient to patient, depending on their blood glucose level.
As a nurse, your key role is to keep the patient informed about their health status and what’s happening inside their body. Make sure to guide them on what’s good and bad for their health, especially when they have diabetes.
As a nurse, explain to the patient the disease process, the goals of management, and strategies to limit complications. Use simple explanations, answer questions, and provide written information for the patient to refer to between teaching sessions.
Along with general information on the disease process, don’t forget to reinforce collaborative teaching about medications and nutrition. The patient also needs specific information about foot care.
In diabetes, foot care remains an important topic as neuropathies lead to loss of sensation in the foot, and the patient can’t sense the blisters or cuts. Being more prone to infections, diabetic patients need to take a lot of foot care as the infection can become life-threatening.
If left untreated, amputation may be needed. Therefore, emphasize to the patient about taking efficient care of their foot health.
Tell the patient that all cuts, abrasions, and blisters should be washed with an antiseptic solution promptly. If they notice a blister that shows signs of infection, such as warmth, pain, and redness, tell them to inform the healthcare provider readily.
Delaying that can complicate the condition. Teach them to avoid wearing constricting clothing, such as constricting stockings, garters, girdles, or elastic slippers.
If the patient needs to be on bed rest, encourage them to keep bed linens loose over the feet and legs. Furthermore, instruct them to avoid having very hot baths as peripheral neuropathy causes decreased temperature sensation.
They might not recognize if their feet get burnt due to hot water. Therefore, it is good to take a bath with mild warm water, not too hot or cold.
If the patient diagnosed with diabetes is a teenager or a child, their family may be in shock and disbelief. Make sure to talk to them and explain things.
For patients with diabetes, their whole life and outlook is changed. Therefore, they need support and counseling.
School-age children may be impressed with the new “condition” and may be challenged by the new skills it involves. In comparison, adolescents may feel unfairly victimized and respond by becoming depressed, resistant, uncooperative, or insecure. Therefore, you have to spend time healing them mentally.
Introduce the family to other families with the same problem and encourage them to talk. However, if you feel the need, refer them to a professional counselor who can look after their mental health well.
Patients dependent on lifelong insulin therapy need to understand its dosage, route of administration, the purpose of administration, and possible side effects. If the patient is to self-administer insulin, demonstrate to them the appropriate preparation and administration techniques. Make sure they are comfortable and have learned the insulin administration properly.
Inform the patient about the complications of diabetes. To prevent them, they should keep their blood glucose levels well under control.
Otherwise, if plasma glucose levels remain elevated for a long time, it can result in serious consequences, leading to heart attack, vision loss, amputation, and life-threatening infections. Inform them they are at increased risk of infections. Moreover, explain to the patients and their caregivers how the complications of diabetes can be prevented.
The following tips can help:

Diabetes is a lifelong condition that needs to be managed well. The patient can continue their daily life activities with medications and insulin. But you have to take more care of the patient as they are at increased risk of infections because of hyperglycemia.
As a nurse, educate the patient about their condition and compel them to attend follow-up visits as diabetes has to be managed lifelong. It can’t be left unattended. Tell them to get their fasting plasma glucose and HBA1c done routinely and get checked by the physician.
Love what you read?
Share our insider knowledge and tips!
Read More

Events | Holidays & Freebies National Nurses Week: Honoring Our Favorite Pop Culture Practitioners National Nurses Week runs from May 6-12, and includes a variety of ways to honor nurses. This year’s theme is “Nurses Make the Difference.” As part...
Events National Cancer Prevention Month February is National Cancer Prevention Month 2024! Nurses can be an educational resource for patients on how to protect themselves. Cancer prevention can look like lifestyle changes to minimize modifiable risk factors and...

Events International Prenatal Infection Prevention Month 2024 February is International Prenatal Infection Prevention Month 2024! Learn about a nurse’s role in educating patients on how to protect themselves. Common prenatal infections you can explore with...